Advances in Animal and Veterinary Sciences
Case Report
Advances in Animal and Veterinary Sciences 2 (4): 239 – 241Therapeutic Management of Camel Pox – A Case report
Subhash Kachhawaha, Mukesh Srivastava*, Jai Prakash Kachhawa1, Mahendra Tanwar1, Ankita Sharma1, Naveen Kumar Singh1, Kapil Kachwaha1, Shravan Singh Rathore1, Ram Kishan Tanwar1
- College of Veterinary and Animal Science, Rajasthan University of Veterinary and Animal Sciences, Bikaner, Rajasthan, India
*Corresponding author: [email protected]
ARTICLE CITATION:
Kachhawaha S, Srivastava M, Kachhawa JP, Tanwar M, Sharma A, Singh NK, Kachwaha K, Rathore, SS, Tanwar RK (2014). Therapeutic management of camel pox– a case report. Adv. Anim. Vet. Sci. 2 (4): 239 – 241.
Received: 2014– 04– 03, Revised: 2014– 04– 11, Accepted: 2014– 04– 12
The electronic version of this article is the complete one and can be found online at
(
http://dx.doi.org/10.14737/journal.aavs/2014/2.4.239.241
)
which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited
ABSTRACT
A camel presented with history of fever, inappetence and development of scab on many part of body along with blindness since more than one week. History revealed suffering of many camels with similar symptom in that area. Clinical examination showed the different stages of pox lesion in the mouth, face, neck, abdominal, thigh region along with lacrimation, corneal opacity in both eyes and enlargement of mandibular lymph nodes. Camel was treated by antibiotic, anti–inflammatory and topical therapy. Animal was successfully managed but without any improvement in the blindness. It was concluded awareness of camel owners about separation of diseased and healthy young camels, improved health care including long acting antibiotics, improved hygiene and general supportive treatment will decrease the harmful effects of camel pox.
Camel pox is a highly contagious, enzootic disease (Duraffour et al, 2011), caused by Orthopoxvirus cameli virus of poxviridae family, which primarily affects young animals (McGrane and Higgins, 1985). It causes benign to severe generalised pox lesions (Pandey et al., 1985), even death in animals less than two years of age or those animals not previously exposed to infection (Munz, 1992). Higher incidence was seen in male with higher mortality rate in young animals (Kritz, 1982). Recorded mortality rate in adult animals is between 5 to 28%, while in young animals it varies from 25% to 100% (Mayer and Czerny, 1990). Clinical manifestations of camel pox range from inapparent and mild local infections, confined to the skin, to moderate and severe infections leading to swelling of whole head (Meena et al, 2012), however, mostly generalised form seen in camels, where pox lesion covers the entire body. The disease is characterised by fever, salivation, lacrimation, mucopurulent nasal discharge, enlarged lymph nodes, diarrhoea and anorexia in the systemic form of the disease and pathgnomonic skin lesions, which appears 1–3 days after the onset of fever. Skin lesions first appear on the head, eyelids, nostrils, margins of the ears and begin as erythematous macules, developing into papules and vesicles, which later on turn to pustules and crusts. In later stage, skin lesions may extend to the neck, limbs, genitalia, mammary glands and perineum. Death is usually due to secondary infections and septicaemia (Wernery and Kaaden, 2002). This variation in clinical manifestation possibly reflects differences between the strains of camel pox (Wernery and Kaaden, 2002). Clinical signs of infected animals are often indistinguishable from lesions caused by parapox (Contagious ecthyma), however, simultaneous infections with both orthopox and parapox viruses have also been described (Renner–Muller et al, 1995; Wernery and Kaaden, 1995). Transmission is by either direct contact between infected and susceptible animals or indirect infection via a contaminated environment. The role of insects in the transmission has been suspected because the disease is often observed after rainfall (Wernery et al,, 1997). Although camel pox virus is very host specific but field reports of mild skin lesions in humans associated with camel pox have been made by Coetzer (2004), underlining that camelpox can be of public health importance (Bera et al, 2011). Present communication reports the clinical manifestation and management of camel pox.
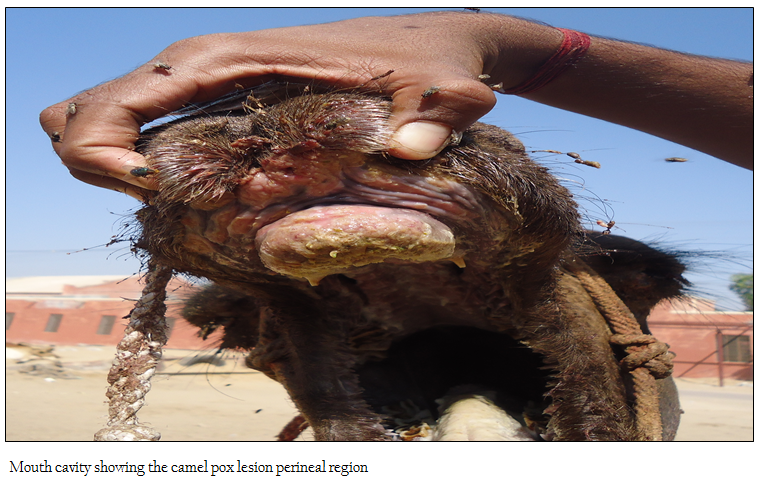
A four years old male camel presented to the Teaching Veterinary Clinical Complex (TVCC), CVAS, Bikaner in the month of September (rainy season), with history of fever, inappetence and development of pustule followed by scab along with blindness since more than one week. History revealed suffering of many camels with similar symptom in that area. Clinical examination showed the different stage of pox lesion in the mouth, face, neck, abdominal, thigh region along with lacrimation and corneal opacity in both eyes (Figure 1), which was developed after 8–10 days of the disease. Mandibular lymph nodes were moderately enlarged but camel neither has any sign of pruritus nor excoriation. There was development of oedema in the dependent parts of the body especially lower limbs and testicles. Routine haematology was unremarkable and inconclusive except mild neutrophilia.
Based on history, clinical examination and in consideration of predisposing factor, differential diagnosis was made for camel pox, contagious ecthyma, papilloma virus and reaction to insect bites (OIE, 2008). As sign were generalised and gradual with pustule and scab, reaction to insect bites was ruled out, also the lesions were not in the form of any growth and morphologically not resembling the papilloma. Clinical differentiation of contagious ecthyma and camel pox was done as suggested by Ademe et al., (2006). Symptom of camel pox include moderate depression, mild fever and anorexia and enlargement of mandibular lymph nodes followed by vesicles that rupture and become covered by thick brown scabs and scar, while contagious ecthyma is clinically characterised by pruritus and itching against objects, followed by haemorrhages and extensive skin excoriations (Ademe et al., 2006). In last, clinical diagnosis was made for camel pox and treatment was initiated with Oxytetracycline @10 mg/kg and Meloxicam @ 0.2 mg/kg body weight for 5 days. Additionally Ciplox eye drop was used to check the eye infection and D–Mag spray containing Gamma benzene hexachloride, Proflavine hemisulphate, Cetrimide, Eucalyptus oil, Turpentine oil and Neem oil (Intas Pharmaceutical) was also use wound management and fly control. This generalised form of the disease is most common form of disease with distribution of lesion on all parts of the body, being first recognised on non hairy part. In the systemic form of the disease, pox lesions can be found in the mucous membranes of the mouth, respiratory and digestive tracts (Kritz, 1982, Wernery and Kaaden, 2002). Identification of infection by molecular biology based diagnostic techniques is best but disease can be diagnosed based on clinical signs. Although there is no specific treatment, but antibiotic therapy is useful to control and prevent secondary bacterial infection (Ademe et al., 2006). As recorded in present case, outbreaks mostly occur during early to middle periods of the rainy season. Similar to present finding, disease mostly occurs in large group of population because;
transmission is by either direct contact between infected and susceptible animals or indirect infection via a contaminated environment. The infection is usually achieved by inhalation or through skin abrasions; also virus is secreted in milk, saliva, and ocular and nasal discharges. Dried scabs shed from the pox lesions may contain live virus for at least 4 months and contaminate the environment. The increased density of the tick population during the rainy season may be responsible for the spread of the disease (Wernery et al, 1997). In dry climates the disease cures itself but in wetter areas, the disease can take severe form. Mortality in calves and immature camels is very high, especially under poor management conditions, but the effects of morbidity may be equally important because they cause heavy production losses, particularly in weight gain. Education of herd owners about the etiology of camel pox, strict separation of diseased and healthy young camels, improved health care including long acting antibiotics, improved hygiene and general supportive treatment will decrease the harmful effects of camel pox (Munz, 1992). The main practical differences between camel pox and ecthyma are that the latter disease is more severe and affects camels of all ages. In ecthyma because of intensive pruritus animals spend a lot of time scratching and rubbing the affected area, resulting in haemorrhages and skin excoriations.
REFERENCES
Bera BC, Shanmugasundaram K, Barua S, Venkatesan G, Virmani N, Riyesh T, Gulati BR, Bhanuprakash V, Vaid RK, Kakker NK, Malik P, Bansal M, Gadvi S, Singh RV, Yadav V, Sardarilal, Nagarajan G, Balamurugan V, Hosamani M, Pathak KM, Singh RK (2011). Zoonotic cases of camel pox infection in India. Vet Microbiol 152:29–38.
http://dx.doi.org/10.1016/j.vetmic.2011.04.010
PMid:21571451
Coetzer JAW (2004). Poxviridae. In: Infectious Diseases of Livestock, Second Edition, Coetzer J.A.W. & Tustin R.C., eds. Oxford University Press, Southern Africa. 2: 1265–1267.
Duraffour S, Meyer H, Andrei G, Snoeck R (2011). Camelpox virus, Antiviral Res, 92(2)167–186.
http://dx.doi.org/10.1016/j.antiviral.2011.09.003
PMid:21945248
Kritz B (1982). A study of camel pox in Somalia. J Compa Path, 92: 1–8.
http://dx.doi.org/10.1016/0021-9975(82)90037-8
Mayer A, Czerny CP (1990). Camel pox Virus. In: Virus Infections of Vertebrates, Vol. 3, Virus Infections of Ruminants, Dinter Z. & Morein B., eds. Elsevier Science Publisher B.V., Amsterdam, Oxford, New York, Tokyo, Chapter 4, 19–22.
McGrane JJ, Higgins AJ (1985). Infectious diseases of the camel: viruses, bacteria and fungi. B Vet J. 141(5) 529–547.
http://dx.doi.org/10.1016/0007-1935(85)90049-1
Meena DS, Mathur M, Dadhich H, Singh AP (2012). Post–mortem observations of camel pox– a case report. JCPR. 19(2):163.
Munz, E (1992). Pox and pox–like diseases in camels. The One–Humped Camel in Eastern Africa. Verlag Josef Margraf, Weikersheim, FR Germany.; 'Proceed First Inter. Camel Conf., pp 43–46. R&W Pub. Limited, Newmarket, Suffolk, United Kingdom
OIE (2008). Camel Pox OIE Terrestrial Manual Chapter 2.9 . 2 . pp–1177–1184.
Pandey R, Kaushik KA, Grover YP (1985). Biology of orthopoxvirus infections of domestic ruminants. Programme Vet Microbiol Immunol. 1:199–228.
PMid:2856166
Renner–Muller ICE, Meyer H, Munz E (1995). Characterisation of camel pox virus isolates from Africa and Asia. Vet Microbiol. 45 (4)371–381.
http://dx.doi.org/10.1016/0378-1135(94)00143-K
Wernery U, Kaaden OR (1995). Infectious diseases of camels. Blackwell Scientific Publications, Oxford, 81–88.
Wernery U, Kaaden OR (2002). Camel pox. In: Infectious Diseases in Camelids, Second Edition, eds. Blackwell Science Berlin, Vienna. 176–185.
http://dx.doi.org/10.1002/9780470699058
Wernery U, Kaaden OR, Ali M (1997). Orthopox virus infections in dromedary camels in United Arab Emirates (U.A.E.) during winter season. JCPR. 4 (1)51–55.